The condition that patients describe to us as brain fog is rarely a single thing. It is, more often, a constellation of symptoms — slowed processing speed, word-finding difficulty, reduced working memory capacity, mental fatigue disproportionate to the cognitive load, a sustained sense of operating one or two steps behind the version of one’s mind that was familiar in earlier years. The patients arriving with these symptoms are not, in most cases, in clinical cognitive decline. They are, however, operating measurably below their previous baseline, and the standard medical pathway frequently has nothing to offer them beyond reassurance and a thyroid panel.
This is one of the more under-served clinical territories in adult medicine. The symptoms are real. The mechanisms are increasingly well-characterised. The interventions that produce measurable improvement are available, but they are not, in most healthcare systems, the interventions that brain fog patients are offered.
This piece outlines what is actually happening in the most common brain fog presentations and what the combination of hyperbaric oxygen therapy and NAD+ infusion therapy can do for them.
What Is Actually Producing the Symptoms
The clinical evidence for HBOT in cognitive recovery is expanding. A 2021 randomised controlled trial published in Aging documented measurable improvements in cognitive function, including memory and processing speed, in adults aged 64+ following a structured 60-session HBOT protocol, with effects associated with telomere lengthening and reduced senescent cell counts.
Brain fog, in the patients we see at Holina Clinic, typically traces back to one or more of several identifiable mechanisms. Neuroinflammation produced by sustained psychological stress, prior infection including the post-viral picture that has become particularly common since 2020, autoimmune activity, or chronic low-grade inflammatory states elsewhere in the body. Mitochondrial dysfunction in neural tissue, reducing the cellular energy available for cognitive work. Reduced cerebral blood flow, sometimes from vascular factors, sometimes from prolonged sedentary lifestyle, sometimes from medications. Suboptimal neurotransmitter function, often related to nutrient status, sleep quality, and hormonal state. NAD+ depletion at the cellular level, which has been increasingly recognised as a factor in age-related cognitive change and in the recovery from various inflammatory and metabolic conditions.
These mechanisms are not mutually exclusive. In most of the patients we work with, two or three of them are operating simultaneously. The standard medical workup tends to identify none of them clearly, because the markers measured in routine bloodwork are not designed to detect the conditions described above. Patients leave their GP appointments with normal results, no diagnosis, and an unchanged condition.
How HBOT Addresses the Substrate
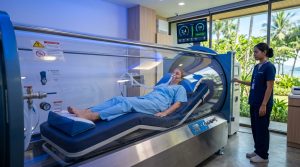
Hyperbaric oxygen therapy delivers oxygen at pressures above atmospheric, dramatically increasing the amount dissolved in plasma and available to tissues that ordinary breathing cannot reach efficiently. For brain tissue specifically, this has several documented effects relevant to brain fog.
Neuroinflammation is reduced. Multiple studies have shown that HBOT modulates inflammatory cytokine signalling in neural tissue, with measurable reductions in markers associated with chronic low-grade inflammation. For patients whose brain fog has an inflammatory component, this is one of the central mechanisms of clinical improvement.
Mitochondrial function is supported. HBOT has been shown to upregulate mitochondrial biogenesis and improve cellular energy production in neural tissue, addressing one of the most common underlying drivers of the fatigue-cognition cluster.
Cerebral blood flow improves, both acutely during the session and durably over a course of treatment, with documented increases in perfusion to regions of the brain involved in executive function and memory.
Stem cell mobilisation occurs systemically during a course of HBOT, with downstream effects on the brain’s capacity for repair and adaptation.
The clinical protocols at Holina Clinic for brain fog presentations typically run 30 to 40 sessions at 1.5 to 2.0 ATA, delivered over six to eight weeks. The dose-response curve is real, and partial courses tend to produce partial results. The full course, in the patients we have worked with, produces sustained improvement in cognitive function that exceeds what any single intervention has been able to deliver.
How NAD+ Therapy Complements HBOT
NAD+ — nicotinamide adenine dinucleotide — is a coenzyme essential to mitochondrial energy production and to the function of the sirtuin family of cellular repair enzymes. Endogenous NAD+ levels decline with age, with chronic inflammation, with metabolic dysfunction, and with prolonged psychological stress. The result, in many adult patients, is a cellular environment in which the substrate for cognitive function is operating well below its potential.
NAD+ infusion therapy delivers the coenzyme directly to systemic circulation, bypassing the limitations of oral precursor supplementation. The clinical effects in brain fog patients include sharper attention, reduced cognitive fatigue, improved word-finding, and a measurable lift in sustained concentration. The effects are typically apparent within the first three to four infusions and consolidate over a full course.
The combination of HBOT and NAD+ produces effects that exceed either alone. HBOT addresses the inflammatory and perfusion substrate. NAD+ provides the cellular fuel for repair and ongoing function. In our clinical experience, the combination is one of the more reliably effective protocols available for adult brain fog.
What the Treatment Course Actually Looks Like
A typical Holina Clinic brain fog protocol begins with baseline assessment — cognitive testing, inflammatory markers, micronutrient and hormonal panels, and where indicated, advanced testing including organic acids and oxidative stress markers. The protocol is then calibrated to the specific picture each patient presents with.
The combined HBOT and NAD+ course typically runs six to eight weeks, with HBOT sessions five days per week and NAD+ infusions twice weekly during the active phase. Patients staying with us at Holina Healing in Khao Yai during this course also benefit from the wider environment — clean food, structured sleep, supportive movement, removal from the stressors that contributed to the substrate. The integrated nature of the setting is part of what produces the clinical results.
Re-assessment at the end of the course documents the changes. For the majority of patients we have worked with, the improvements are substantial and sustain beyond the active treatment phase, particularly when the lifestyle factors that contributed to the original condition are addressed during the residential window.
Who This Protocol Is Appropriate For
Adults presenting with brain fog disproportionate to age and lifestyle. Patients in the post-viral recovery picture who have not returned to cognitive baseline. Patients with chronic inflammatory conditions whose mental sharpness has progressively declined. Patients with autoimmune conditions managed medically whose cognitive symptoms have not responded to the underlying disease management. Adults whose cognitive function has declined alongside hormonal transitions and whose hormone replacement, where appropriate, has produced incomplete recovery. Patients recovering from extended illness, surgery, or major medical events whose cognitive function has not fully returned.
The protocol is less appropriate as a first-line intervention for patients with active major depressive disorder, untreated thyroid disease, untreated sleep apnoea, or other conditions where the brain fog is a symptom of a more proximate cause that requires direct treatment. In these cases, the underlying condition is addressed first, and the protocol is considered if cognitive symptoms persist.
A Closing Note
If you have been told that your bloodwork is normal and the brain fog is something to live with, the standard workup has not, in most cases, examined the substrate where the actual condition is operating. The work that addresses it is available. The first conversation with our clinical team is the beginning of finding out what your specific picture looks like and what the appropriate protocol for it would be.