The patient arrives having read the sleep hygiene materials. Most have tried the lavender, the white noise, the blue light filters, the meditation apps, the magnesium powder, the careful avoidance of screens after nine. Some have taken the over-the-counter melatonin, sometimes for years. A meaningful proportion have, at some point, been prescribed a short course of a sedative or a sedating antidepressant, and most have either not tolerated these or have not wanted to continue beyond the brief window the prescribing clinician was comfortable with. None of this has, in the patient’s experience, produced the sleep that they remember having before whatever year their sleep first changed.
This is one of the most common presentations we see at Holina Clinic, and it is one of the most under-treated conditions in adult medicine. The patients are not exhibiting acute sleep disorders that the standard pathway is designed for. They are exhibiting the more diffuse, chronic, mechanistically complex sleep dysfunction that the generic advice has not addressed because the substrate driving it is not what the advice assumes.
This piece outlines what the actual mechanisms of adult sleep dysfunction tend to be and what a clinical optimisation protocol involves.
Why Generic Sleep Hygiene Often Fails
The scale of adult sleep dysfunction is substantial. US CDC data consistently finds that approximately 1 in 3 adults regularly fails to get the recommended amount of sleep, with chronic sleep deprivation linked to elevated rates of cardiovascular disease, metabolic dysfunction, depression, and cognitive decline.
The standard sleep hygiene literature assumes a substrate that is mostly functioning, with surface behaviours that need correction. For adults whose substrate is functioning, the standard advice can be sufficient. For adults whose substrate has progressively dysregulated over years of stress, hormonal change, inflammation, and metabolic shift, the advice does not reach the actual condition.
What is happening in these patients, in most cases, is a combination of mechanisms operating together. Cortisol rhythm disruption, with elevated evening cortisol delaying sleep onset and early morning awakenings producing fragmented sleep. Melatonin production deficits, often related to inflammation, light exposure patterns, or age-related decline. Autonomic dysregulation, with the parasympathetic nervous system unable to dominate during the evening transition. Disrupted core body temperature regulation, which is one of the central physiological signals that the sleep system relies on. Suboptimal blood sugar regulation overnight, producing hypoglycaemic micro-awakenings the patient does not consciously remember. Sex hormone shifts, particularly in perimenopausal and menopausal women but also in men with declining testosterone. Subclinical inflammation that disrupts sleep architecture even without producing recognisable acute symptoms.
These mechanisms are not detected by the standard medical workup. Patients with the picture described above typically have unremarkable bloodwork and are told that their sleep difficulty is functional. The functional framing is partly correct — the condition is not pathological in the structural sense — but it is also not what current medicine has frameworks to address.
What Comprehensive Clinical Assessment Looks Like
At Holina Clinic, the assessment of chronic adult sleep dysfunction begins with detailed history that goes beyond what a brief sleep clinic appointment typically captures. The temporal pattern of when the sleep changed, what was happening in life and health at that point, how the sleep is dysfunctional now in specific ways, what has and has not helped over the intervening period.
Laboratory work includes diurnal cortisol assessment through salivary or urinary measurement at multiple time points, sex hormone panels appropriate to age and sex, comprehensive inflammatory markers, micronutrient status including vitamin D and magnesium, and where indicated, advanced testing for organic acid metabolism, neurotransmitter precursors, and overnight glucose patterns.
Where appropriate, formal sleep architecture assessment through home sleep studies or polysomnography is arranged to identify any underlying sleep-disordered breathing, periodic limb movements, or specific architectural patterns that require direct treatment.
The picture that emerges is typically a multi-factor one. The protocol is then calibrated to what is actually driving the dysfunction.
The Protocols We Use
The interventions that produce reliable improvement in chronic adult sleep dysfunction draw on several modalities working together.
Circadian rhythm restoration is the foundation. This involves more than the standard advice. We use specific timed light exposure, often supported by clinical-grade light therapy devices, calibrated to the individual’s circadian pattern. We address evening cortisol elevation through specific behavioural protocols and, where indicated, supportive interventions including phosphatidylserine and ashwagandha at clinical doses.
Melatonin optimisation involves more than the typical over-the-counter approach. Low-dose, sustained-release, timed-release, and combination formulations all have different clinical applications, and the protocol is matched to the picture. For some patients, this involves prescription-strength melatonin formulations not widely available in standard pharmacies.
Hormonal optimisation, where appropriate, addresses the perimenopausal, menopausal, or andropausal substrate that is often a central driver. This is undertaken in coordination with the patient’s existing endocrinology or gynaecology care where present.
Nutritional protocols address the substrate. Magnesium glycinate or threonate at clinical doses. Glycine. Targeted amino acid support where neurotransmitter precursor deficits are documented. Overnight blood sugar stability through evening protein and fat distribution.
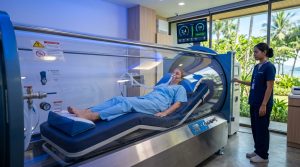
Hyperbaric oxygen therapy, where the picture includes inflammatory or post-illness components, can shift the substrate substantially. The effects on sleep architecture from a structured HBOT course are well-documented in the relevant literature.
NAD+ infusion, where the picture includes mitochondrial or metabolic substrate, can produce measurable improvement in sleep quality alongside its broader metabolic effects.
Cognitive-behavioural therapy for insomnia, where appropriate, addresses the cognitive and behavioural patterns that often develop over years of poor sleep and become drivers of the dysfunction in their own right.
The combined protocol is typically delivered over six to twelve weeks, with reassessment at the end and continued adjustment based on response.
Who This Is For
Adults whose sleep dysfunction has persisted for more than a year despite reasonable lifestyle interventions. Patients in perimenopausal or menopausal transition whose sleep has not responded adequately to hormone replacement alone. Patients with chronic inflammatory or autoimmune conditions whose sleep has progressively worsened. Patients in post-viral recovery whose sleep architecture has not returned to baseline. High-functioning adults whose careers and lives have continued but whose sleep quality has been substantially below their previous baseline for years. Patients who have tried multiple medications for sleep and either not tolerated them or not been willing to remain on them indefinitely.
The protocol is less appropriate as a first-line intervention for acute sleep difficulty in the first weeks after a clear precipitating event, for patients with untreated obstructive sleep apnoea where direct treatment is required, or for patients in active acute psychiatric illness where the underlying condition needs primary attention.
A Closing Note
If you have been managing chronic sleep dysfunction for years through accumulating workarounds that have not produced restoration, the substrate that the generic advice does not reach is, in most cases, the substrate that requires attention. The clinical work that addresses it exists, has identifiable mechanisms, and produces measurable improvement in the quality of sleep and the quality of the days that follow it. The first conversation with our clinical team is the beginning of finding out what your specific picture is and what protocol would address it.