The advice has been roughly the same for years. Better sleep. More exercise. Reduce caffeine. Manage stress. Improve diet. These are reasonable interventions, and for adults whose energy levels have declined as a downstream consequence of suboptimal lifestyle, they are typically what is required. For a meaningful proportion of the patients arriving at Holina Clinic with persistent fatigue, however, the lifestyle interventions have been tried, sometimes for years, and the underlying condition has not responded. The patient has been told, by various clinicians along the way, that the bloodwork is normal, that the symptoms must be related to stress, that perhaps an antidepressant could be considered. None of this has, on closer examination, addressed what is actually happening.
What is actually happening, in a substantial proportion of these patients, is mitochondrial dysfunction — a reduced capacity at the cellular level for the energy production that all physiological function depends on. The condition has specific mechanisms, identifiable markers, and interventions that produce measurable improvement. It is also, in most healthcare systems, not what the standard pathway is structured to identify or address.
This piece outlines what mitochondrial dysfunction actually is, what produces it, how to assess it, and what the protocols at Holina Clinic can do for it.
What Mitochondria Actually Do
NAD+ decline is one of the better-characterised features of biological ageing. Research summarised in Nature Reviews Molecular Cell Biology documents that NAD+ levels decline substantially with age and in multiple chronic disease states, with restoration through precursor supplementation or direct infusion producing measurable improvements in mitochondrial function in clinical studies.
Mitochondria are the cellular organelles responsible for converting nutrients into adenosine triphosphate — ATP — the molecule that powers virtually every active cellular process in the human body. The brain, the heart, the muscles, the immune system, the digestive system, the endocrine system all depend on adequate mitochondrial function for their operation. When mitochondrial function declines, the downstream effects are systemic. Energy levels reduce. Cognitive function diminishes. Exercise tolerance falls. Recovery from minor illness slows. The immune system operates less efficiently. Hormonal balance becomes harder to maintain.
The clinical picture this produces, in adult patients, is the constellation that most fatigue patients describe. Persistent tiredness disproportionate to recent activity. Post-exertional fatigue that exceeds normal recovery. Cognitive slowing, particularly under demand. Reduced exercise capacity. Slow recovery from minor infections. A felt sense that the body is operating on a reduced budget that the lifestyle changes alone are not increasing.
What Causes Mitochondrial Dysfunction
Multiple factors contribute, often simultaneously. Chronic inflammatory states, whether from autoimmune conditions, chronic infection, or sustained psychological stress, impair mitochondrial function over time. Environmental toxicant exposure — heavy metals, persistent organic pollutants, mould toxins — directly damages mitochondrial membranes and disrupts function. Nutrient deficiencies in cofactors essential to mitochondrial function, particularly B-vitamins, magnesium, CoQ10, and L-carnitine, reduce the substrate available for energy production. Age-related decline in NAD+, the coenzyme central to mitochondrial energy production, progressively reduces capacity. Prior infections, including the picture commonly described in long COVID, can produce sustained mitochondrial impairment that persists long after the active infection has resolved. Medications including certain statins, some antibiotics, and several psychiatric medications have mitochondrial side effects that are often unrecognised in standard prescribing.
In most patients we work with, two or three of these factors are operating together. Identifying the specific contributors is part of the clinical work, because the protocol is calibrated to what is actually driving the picture rather than applied generically.
How We Assess Mitochondrial Function
Standard medical bloodwork does not assess mitochondrial function. The tests that do are available through specialist functional medicine laboratories and include organic acid testing for markers of mitochondrial output and substrate utilisation, oxidative stress markers, fatty acid metabolism panels, and assessment of micronutrient status at the cellular level rather than the serum level. Where appropriate, we also assess for environmental toxicant burden through urinary and serum measures.
Alongside the laboratory work, careful clinical history is essential. The pattern of fatigue, its temporal evolution, its relationship to specific exposures or events, the response to prior interventions — all of these inform the picture and the protocol that addresses it.
The Interventions That Address Mitochondrial Dysfunction
The protocols at Holina Clinic for mitochondrial dysfunction are individualised but draw on a recognised range of effective interventions.
NAD+ infusion therapy directly addresses the coenzyme depletion that is one of the central features of the condition. Delivered as an IV protocol typically over several weeks, NAD+ produces measurable improvements in cellular energy production, cognitive function, and exercise tolerance in patients whose mitochondrial picture includes this depletion.
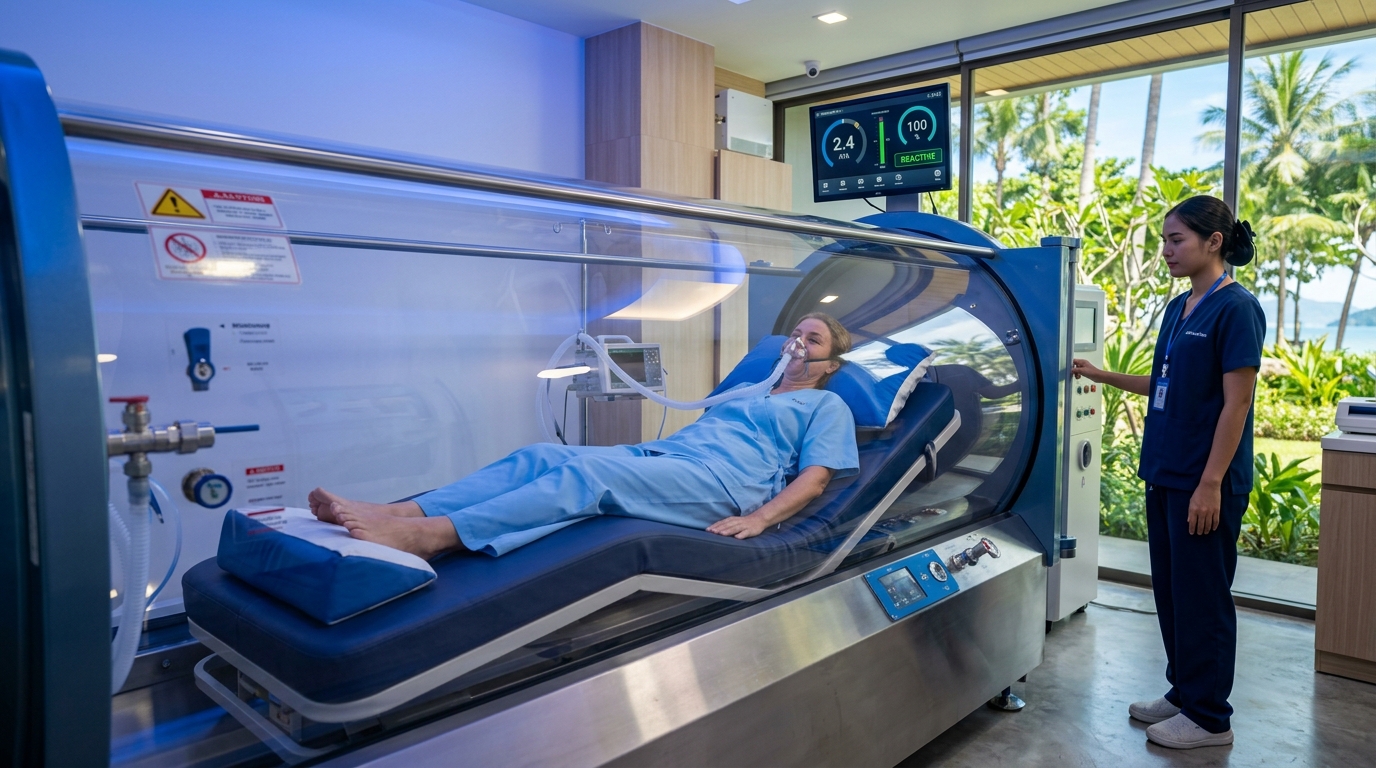
Hyperbaric oxygen therapy supports mitochondrial biogenesis, the cellular process by which new and healthier mitochondria are produced. A structured HBOT course can substantially shift the mitochondrial population of cells toward more functional capacity, with effects that persist beyond the active treatment window.
Targeted micronutrient correction addresses the substrate deficiencies that have been limiting mitochondrial function. This is done through IV protocols where indicated and through carefully calibrated oral supplementation matched to the laboratory picture. Generic high-dose supplementation without testing is generally not what is required and can occasionally be counterproductive.
Identification and addressing of environmental toxicant burden, where this is part of the picture, is undertaken through specific detoxification protocols matched to the toxicant involved. Heavy metal protocols are different from mould protocols are different from persistent organic pollutant protocols, and the work is calibrated accordingly.
Sleep optimisation, structured movement, and dietary work address the lifestyle substrate that supports the cellular work. These are not the centre of the protocol, but they are essential supporting structure.
What Recovery Looks Like
For patients with mitochondrial dysfunction whose condition responds to the integrated protocol, recovery is typically gradual and measurable over a course of treatment. Energy levels improve, often substantially. Cognitive function clears. Exercise tolerance returns. The reduced functional capacity that has been organising the patient’s life for some years begins to expand.
The pacing matters. Mitochondrial work is not a rapid intervention. The cellular machinery takes time to recover, and the protocol is delivered over weeks to months rather than days. Patients who attempt to compress the work, or who push back into high activity before the recovery has consolidated, frequently experience setbacks. The protocol is designed around what the cellular biology actually requires.
Who This Is Appropriate For
Adults with persistent fatigue not adequately explained by standard workup. Patients with post-viral fatigue syndromes including long COVID. Patients with chronic fatigue syndrome and ME/CFS where mitochondrial mechanisms are documented or suspected. Patients with chronic inflammatory or autoimmune conditions whose fatigue persists despite adequate disease management. Patients recovering from extended illness, surgery, or major medical events whose energy levels have not fully returned. Patients with documented environmental toxicant burden affecting cellular function.
The protocol is less appropriate as a first-line intervention for patients whose fatigue is driven primarily by untreated sleep disorders, major depressive disorder, or other conditions that require direct treatment first. These are addressed in pre-protocol assessment.
A Closing Note
If you have been told that your fatigue is a lifestyle problem and the lifestyle adjustments have not produced the improvement you were promised, the substrate that the standard advice does not reach is, in many cases, the substrate that actually requires attention. The work that addresses it exists, has identifiable mechanisms, and produces measurable results. The first conversation with our clinical team is the beginning of finding out what your specific picture looks like and what the appropriate protocol for it would be.